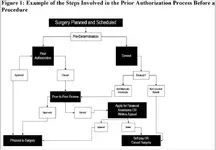
A Plastics provider with my group is OON with most insurances. He’s frequently called to perform intraoperative closures on scheduled surgical cases by other providers of different specialty. All his claims are being denied for no auth, I’ve tried to submit medical records citing it was an intraop procedure, but the denials get held. Any advice on how to dispute this would really help. TIA!
-

Register to Access the Free Forums and 3 Free CEUs!
To view the content for the 3 free CEUs, please sign up today.
CLICK HERE TO REGISTER -
The CCO Community is Moving to Circle!
Click Here to Read More -

Missing Access To A Course, Blitz or Exam? Have Technical Issues? Open a Help Desk Ticket
Please Do Not Post in the Community About Access or Technical Issues
CCO Business Hours for Help Desk and Coaching: Mon-Fri 9am-4pm Eastern
OON Provider Performing Intraop Procedures
- Thread starter JuliaS_81202
- Start date